Toxic Water, Part II
Further fueling the quest for clean water, the foul quality of Manhattan’s water supply caused epidemics of yellow fever (the first of six epidemics killed nearly six percent of the population) and cholera. (The cholera outbreak was caused by the bacterium Vibrio cholerae, often found in contaminated water.) On June 26th, 1832 the first cholera outbreak struck Manhattan. Wealthy New Yorkers fled to the country to avoid infection (about one third of the population), leaving mostly immigrants and low-income families. More than 3,500 people died, with the first of many deaths in the Five Points neighborhood (current day Foley Square and Chinatown), where many Irish-Catholic immigrants and African Americans lived. The need for a new supply of fresh water for residents was crucial.

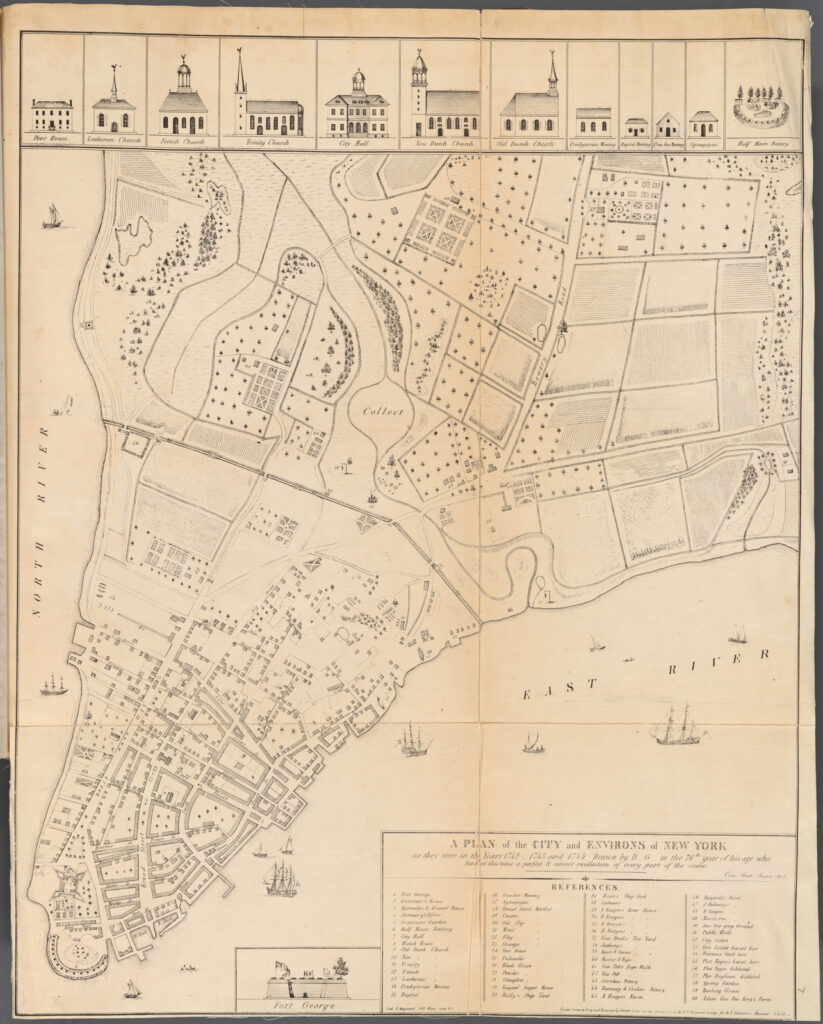
At the time of the early yellow fever outbreaks, New York physician Valentine Seaman created a map of cases in lower manhattan. This blog does a good job explaining Seaman’s work and the geographic nature of the outbreak in New York.
This map “illustrates the environmental history for the section of New York City north of the urban setting. Large farming areas are established, meaning that most of the surface water is due to lowland seasonal wetland field settings, along with a number of flowing brackish waterways, small streams, rivulets, canals and seasonal water ways. The edge of the terrain consists mostly of brackish or mixed fresh-salt water environmental settings, and was rich in sedges, reeds, rush, cattails, phragmites and arundinaria. The related zoology of this setting would make it very likely to be a primary source of the miasma or effluvium so often related to diseases. Anybody residing within 1000 feet from these places would consider his or her residence very susceptible to exposure to these natural causes for fever. Close to the source for this malaria there was the Collect Pond with its long passageway to the East River. This ecological setting was prime territory for mosquito-born diseases. For this reason it is possible this setting experienced occasional malaria, typhoid, or even yellow fever like problems. But the placement of the wetlands needed to harbor these vectors would have been located wither within the natural terrain settings or at the water edge of the urban region, the precursors to the ports built by the 1790s.”
From brianaltonenmph.com
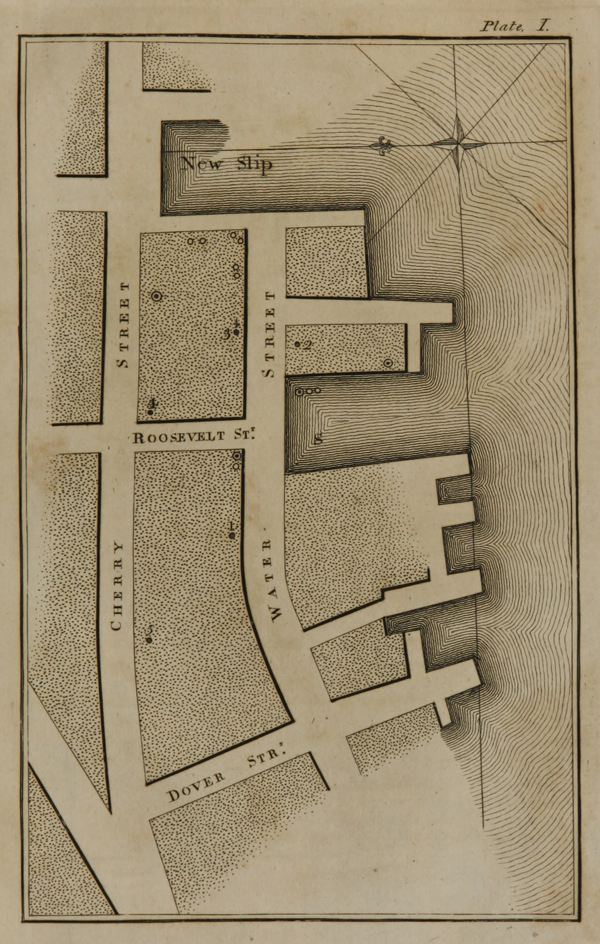

Above, Valentine Seaman’s maps of the yellow fever epidemic in New York City, 1798. Seaman’s maps mark cases of yellow fever. He sorted the cases into three categories: yellow fever, yellow fever-like, those who were as a group taken ill.
Source: Wikimedia Commons. Excerpt from ‘An inquiry into the causes of the prevalence of the yellow fever in New York’ by Valentine Seaman. Full text via Internet Archive.
“Yellow fever came to the Americas from Africa, carried by slave ships that docked in the West Indies. Water barrels on board provided an ideal breeding ground for the Aedes aegypti. Over time, as trade routes expanded, yellow fever reached North America’s eastern ports.”
“The fact that shipborne mosquitos thrived along the waterfront was not then a matter of concern. The very idea that a tiny vector like the Aedes aegypti could cause such an immense catastrophe was simply beyond scientific understanding. Still, what is striking about the writings of New Yorkers in the summer of 1795 is their constant notice of mosquitos…”
From Bellevue: Three Centuries of Medicine and Mayhem at America’s Most Storied Hospital by David Oshinsky. (p 15-17)

“The spring-fed body of water near Canal Street called the Collect, or Fresh Water Pond, was known for its “great depth and unusual purity.” Once a center for ice-skating and shoreline picnics, the Collect would become one of Manhattan’s first ecologic casualties—a dumping ground for dead animals, rubbish, and factory waste. Too dangerous to drink, a place of “insufferable stench,” it was filled with dirt and carved up for residential use. On this landfill rose the infamous slum known as Five Points.”
“In 1832, cholera came to Five Points. It arrived during a lull in the city’s ongoing struggle against epidemic disease… An intestinal disease, cholera spreads when food and water are contaminated with the excrement of infected victims. The bacterium responsible, Vibrio cholerae, causes the body to expel huge quantities of liquid…”
“Cholera in the United States is a distant memory, though it remains a serious threat in the developing world. Effective sewage systems, chlorinated water, powerful drugs, better hygiene—all played a role in its demise.”
“Five Points did suffer higher rates of cholera for reasons all too clear. First, there was no means of escape. The people were too poor to pack up and leave when an epidemic occurred, unlike wealthier New Yorkers who fled the city in droves… Second, these immigrants had no choice but to use whatever water was at hand. In Five Points, that meant a series of shallow wells polluted by fecal waste from backyard privies. Rich folk could drink for purer sources. Some even paid to have fresh water carted in from lakes and springs north of the city—not because they feared contamination, but because it tasted better. That simple preference likely saved their lives.”
From Bellevue: Three Centuries of Medicine and Mayhem at America’s Most Storied Hospital by David Oshinsky. (p 39-41)
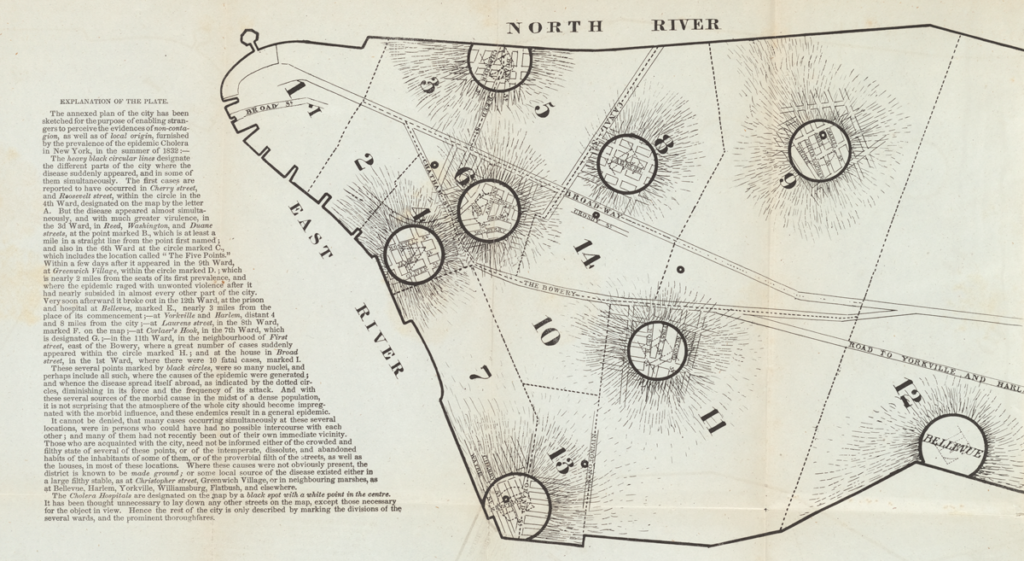
“Epidemics can be tricky as agents of change. They arrive with frightening force, do their awful damage, and leave as mysteriously as they come. It’s easy to view them as freaks of nature, or divine occurrences, impossible to control. In the case of cholera, however, some valuable lessons would be learned… Three years later [after 1832], New Yorkers approved the construction of a forty-one-mile-long aqueduct to bring clean water from the Croton River, north of the city…The project, costing $11.5 million and employing four thousand workers, allowed the city to slowly phase out its hodgepodge of contaminated wells.”
From Bellevue: Three Centuries of Medicine and Mayhem at America’s Most Storied Hospital by David Oshinsky. (p 44)
Further Reading
Cholera, Centers for Disease Control and Prevention
Yellow Fever, World Health Organization
“Coronavirus: New York’s built environment was shaped by pandemics,” by James Nevius in Curbed, 2020.
Article noting the resonance of the cholera epidemic and the AIDs epidemic: “How Epidemics Helped Shape the Modern Metropolis,” by John Noble Wilford, The New York Times, 2008.


